Read OPA’s op-ed on the Canadian Healthcare Network.
Check out OPA’s op-ed on Healthy Debate.

As Ontario marks one year of its Primary Care Action Plan, the Ontario Physiotherapy Association (OPA) is calling for a critical shift in how we talk about healthcare professionals. Stop using the term “allied health” and start naming the specific expertise that matters.
OPA leadership argues that lumping physiotherapists and other regulated health professionals under the umbrella term “allied” obscures their critical role in Ontario’s healthcare system and the patient outcomes they deliver. With over 275,000 Ontarians newly attached to primary care in just one year, the province is on track to meet ambitious targets. But truly integrated care requires recognizing physiotherapists not just as supporting players, but also as frontline providers who diagnose, manage, and treat musculoskeletal and neurological conditions every single day.
A recent physician-authored op-ed questioned physiotherapists’ authority to order diagnostic imaging which is a scope expansion already approved in Ontario’s legislation. It has also been successfully implemented in other jurisdictions including the UK, Australia, and several Canadian provinces. Evidence shows that when physiotherapists have this authority, they order less imaging and reduce unnecessary pain medication. Despite this, Ontario has yet to enable this change.
With Ontario’s health system under mounting pressure from population growth, aging demographics, and complexity, the province needs physiotherapists working at their full scope of practice. That means removing artificial barriers, enabling evidence-based scope of practice expansion, and most importantly, calling these professionals by name.
Read the full op-ed below.
Going Beyond ‘Allied’: The Critical Role of Physiotherapists in Ontario’s Primary Care System
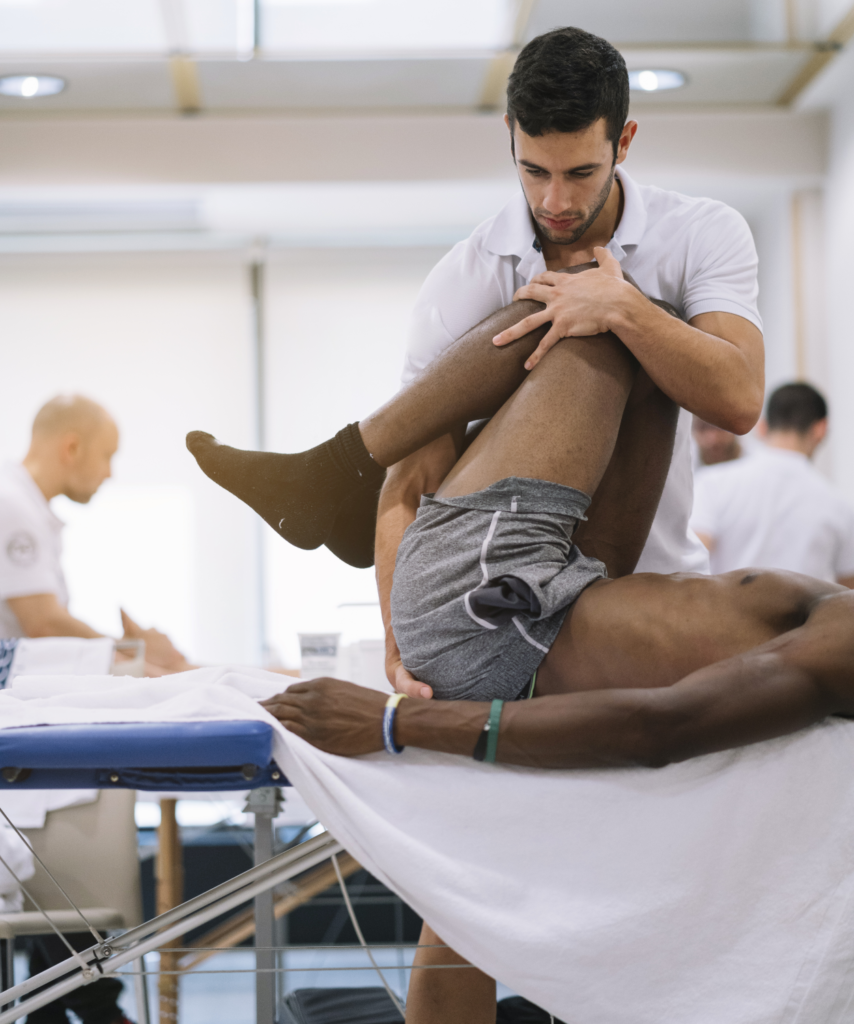
Just say their name – Physiotherapists
I was struck this past week as the one-year milestone of Ontario’s Primary Care Action Plan was announced. The Ontario government noted progress in attaching patients to a primary care provider and how much work there is left to do in expanding the definition of ‘primary care’ and the role of ‘allied health professionals’ in inter-professional care teams and beyond. While I applaud the progress made to date, the use of the word ‘allied’ is a source of increasing frustration for me. It obscures the potential contribution of each of the health professionals who are referred to in this group.
Let me explain.
Physiotherapists are regulated health professionals. Patients don’t need a referral to access a physiotherapist, and where one is requested, it is usually the requirement of an insurance company. Physiotherapists work across the health system, in communities, in hospitals, in primary care, in homecare and in long term care, providing evidence informed care to treat a wide range of musculoskeletal (MSK), cardiorespiratory and neurological conditions. They are patient centric professionals dedicated to restoring movement and function, alleviating pain, and improving quality of life for those recovering from an injury, managing a chronic condition, requiring pre- and post-surgical care, or seeking to improve physical health and well-being.
For many seniors access to physiotherapy by regulated physiotherapists impacts mobility, overall function and the ability to live independently. For MSK conditions, physiotherapists are often the first point of contact and they assess, diagnose, and manage these conditions each and every day. They work both independently and as a member of an interprofessional care team, in a myriad of settings.
Enable Full Scope of Practice in Ontario
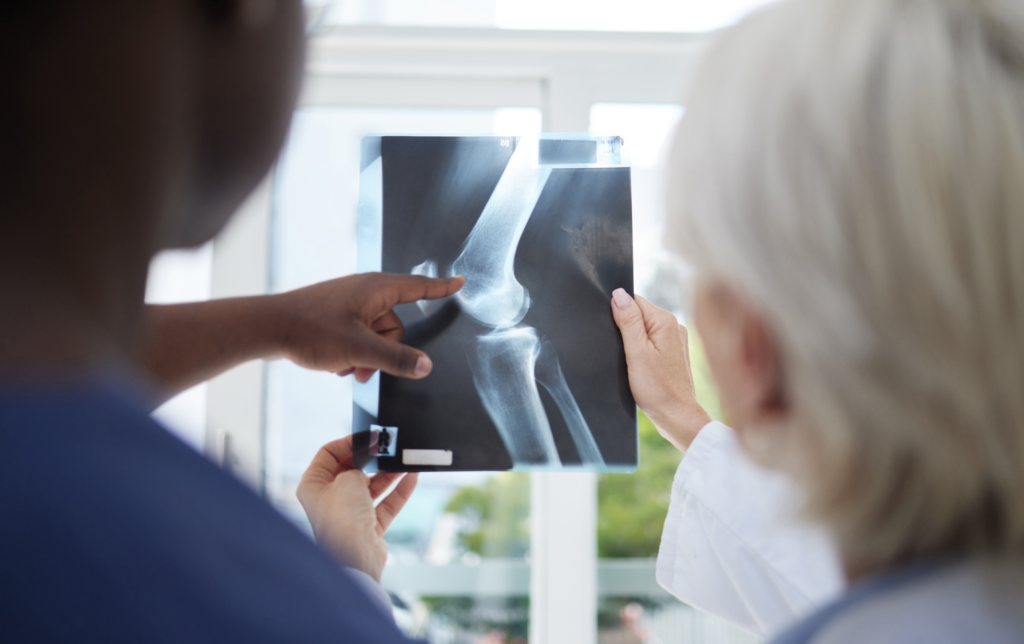
In fact, if the scope of practice changes already approved in Ontario legislation in 2009 are enabled in 2026, physiotherapists would be able to order diagnostic tests. This would increase timely access to care and provide a more seamless patient experience.
Enabling physiotherapists to practice at their full scope will:
- reduce the number of contact points needed within the health system
- reduce inappropriate utilization of walk-in clinics or emergency departments for imaging referrals
Patients would get appropriate and comprehensive care where and when they need it. Truly integrated care means that a qualified professional can act in the patients’ interest to provide care without artificial barriers or any additional gatekeeping. With a patient centered lens, this could mean potential earlier return to function for patients, including care of self, family and earlier return to work. There would be potential savings for employers with improved time to return to work, reduced expenses related to travel and to eliminated healthcare visits. After all, this is about patients.
Important Role of PTs in Ordering Diagnostic Imaging
Recently a newspaper article published by two physician authors questioned the role of physiotherapists in ordering diagnostic imaging suggesting that this would cause new problems and delay access to MRIs. Their statements were not based in evidence and drew a robust factual response from OPA member physiotherapists citing the evidence. Published studies demonstrate that first contact physiotherapists order less imaging and reduce the need for prescription pain relief. It is unfortunate that Ontario has not followed the lead and the evidence from other jurisdictions (UK, Australia, QC, AB and PEI) where this authority exists. Although, we remain hopeful that before the second anniversary of the Primary Care Action Team this will finally have advanced.
Our health system continues to buckle under the demands; whether that’s population growth, population distribution in the province, our aging population or the complexity in navigating our health system of systems. We need more physiotherapists working to full scope of practice to meet these grown demands. We would prefer to have ‘allies’ enacting system change who understand the value and impact that access to physiotherapy across the continuum of care has for patients in our province. Finally, let us name and respect the contribution of all of those “allied” health professionals that make a tremendous impact of the health and well-being of Ontarians.
Sarah Hutchison, MHSc., LL.M, ICD.D
Chief Executive Officer, Ontario Physiotherapy Association





