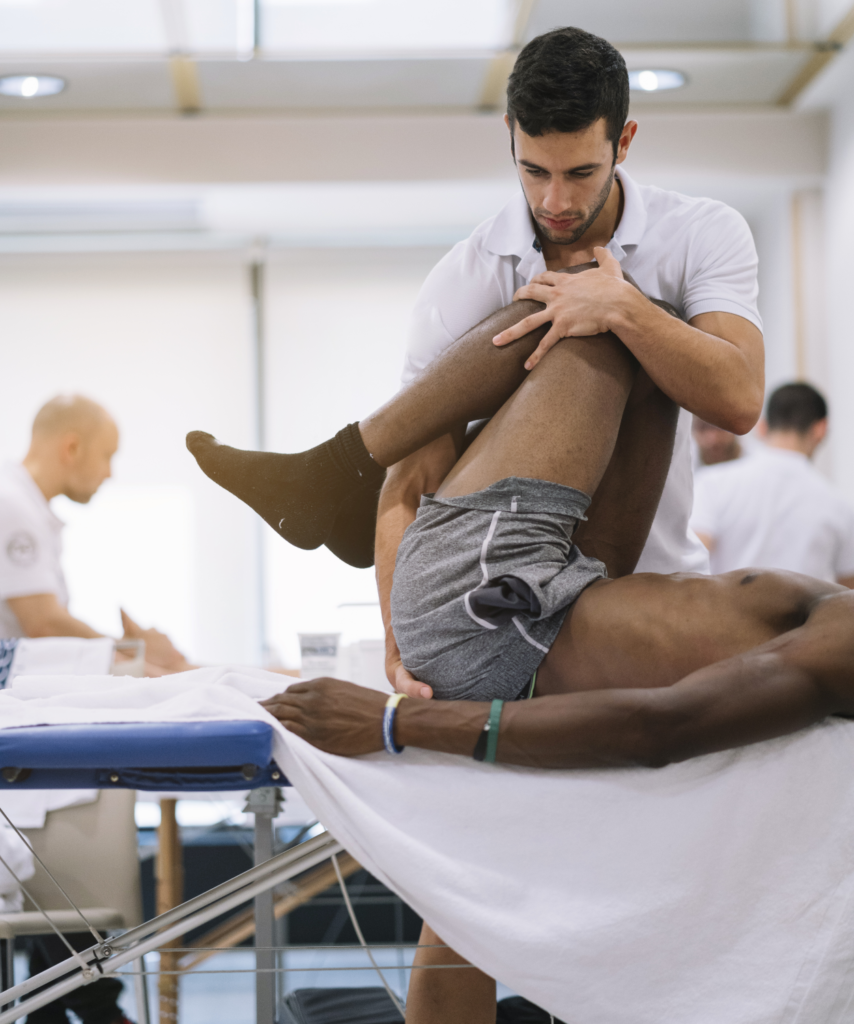
Makaila Koshurba and Riley Pedulla are dedicated physiotherapists working in emergency departments (EDs) in Ontario. Their work is critical to reducing the burden on physicians in the Emergency Department, and their work also benefits patients who need physiotherapy.
Once assessed and treated, Makaila and Riley often refer patients to publicly funded physiotherapy clinics in the community, called Community Physiotherapy Clinics (CPCs), for follow-up care. Makaila and Riley see every day how critical it is to have publicly funded physiotherapists both in the ED and in the community.
“As physiotherapists (PTs) in the ED, we know from firsthand experience the benefits of Community Physiotherapy Clinics. Daily, we assess and treat patients who benefit significantly from physiotherapy follow-up in the community. These patients often cannot afford private physiotherapy services and are referred to a CPC when eligible. Funding stagnation of the CPC program puts a large population at risk of losing access to essential care.
CPCs prevent 70,000 ED visits annually and lack of support for the program risks increasing the burden on EDs as these patients return seeking answers to questions about their diagnosis, rehabilitation, and return to function.”
Despite a proven track record that Community Physiotherapy Clinics reduce strain on the healthcare system, the Ontario government recently notified CPCs that there will be no change to patient funding or program capacity over the next two years. CPCs are already underfunded and at capacity: this lack of investment is increasingly compromising access to care for those patients who need it the most.
CPCs reduce visits to primary care, emergency departments (EDs), specialists, and prevent acute care admissions. This dearth of funding puts our patients and clinics at risk as service provision cannot keep up with patient needs. The CPC funding issue creates a large gap in the continuum of physiotherapy services from acute care to community-based care.
Physiotherapists are Also Needed in Every Emergency Department
There is a significant opportunity to ensure PTs are placed in all EDs across the province as well, and to utilize the PT scope of practice to the fullest extent. For many patients, especially those without private health insurance or access to publicly funded services, ED-based physiotherapy may be their only timely, affordable option for physiotherapy care.
“In our experience, both patients and physicians have called the patient-centred, compassionate, and comprehensive approach that physiotherapists provide an essential part of healthy recovery.”
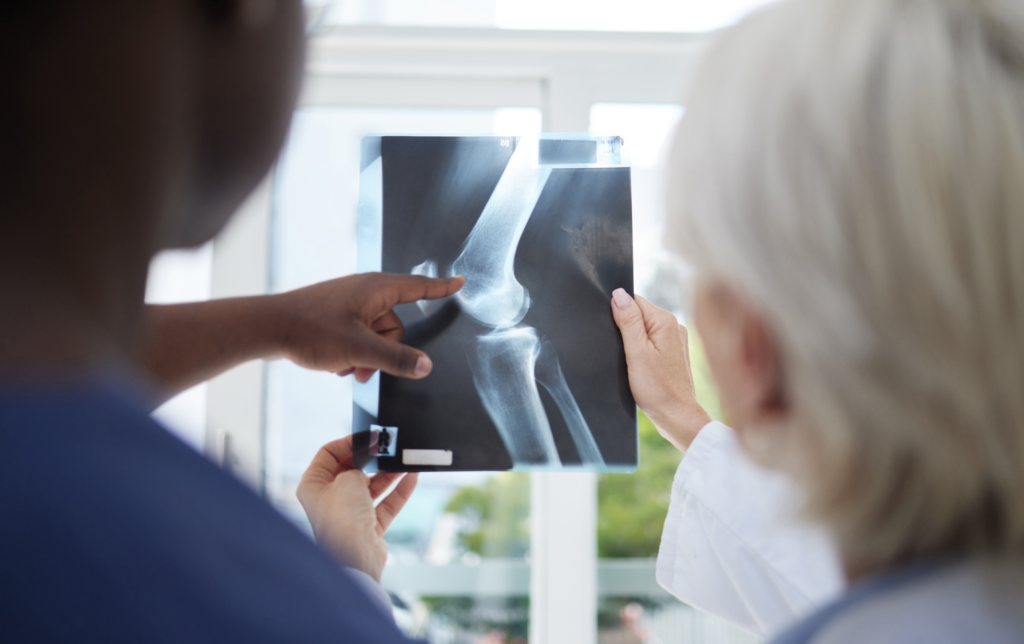
Physiotherapists help patients feel more confident at discharge and help physicians by tackling cases that require more support than can usually be provided in busy EDs. Patients who see ED physiotherapists receive non-pharmacological pain management strategies, clarity about their prognosis and diagnosis, and activity modifications to help them return to the community.
Increasingly, Ontario EDs have physiotherapists who assess and manage care for patients presenting with cardiorespiratory, neurological, and/or musculoskeletal (MSK) complaints. ED PTs see a variety of patients ranging from elderly people with hip fractures to young athletes worried about a concussion, and everything in between.
Growing evidence supports the integration of physiotherapy in EDs highlighting significant benefits such as reduced wait times, improved patient satisfaction, and potential cost savings (Ocampo-Chan & Levy, 2025). However, not all Ontario EDs have physiotherapists, and not all physiotherapy care models in EDs are the same.
CPCs Essential for Preventing Emergency Visits and Future Injuries
A key part of the physiotherapist’s ED role is also to direct patients to the appropriate follow up care. However, without a reliable follow-up point of care like the CPCs, Makaila and Riley anticipate a higher rate of return to emergency departments for this patient population. The importance of CPC programming cannot be understated. Patients seen in the ED benefit from access to CPCs to continue their care, fully rehabilitate, and prevent future injuries. The budget silence on CPC is not just a physiotherapy issue; it negatively impacts the residents of Ontario, their local EDs, and ultimately burdens an already strained system.
CPCs have been a staple in community care and continue to provide people in Ontario with essential services. Program funding should reflect the indispensable nature of the services provided. Furthermore, dedicated physiotherapists should also be available in every Ontario ED.
Take Action Now
We ask that our physiotherapy colleagues support OPA’s advocacy by signing the petition in response to the CPC funding crisis.
We also ask that those working in an acute care setting consider whether their ED has dedicated physiotherapy coverage, and if not, to consider advocating for it. It is time that our staffing models, funding structures, and our government catch up to what the evidence and our patients have been telling us for years.
Sign OPA’s Petition
OPA continues to advocate for the Government of Ontario to reconsider their decision to provide no increases to funding or capacity in the CPC program. Join our advocacy by signing our petition, write your local MPP or sign your name to our letter to Premier Doug Ford and Minister of Health Sylvia Jones. Contact OPA with any questions.
About Makaila and Riley
Makaila Koshurba and Riley Pedulla are Registered Physiotherapists working in urban EDs. They are passionate about healthcare quality, health equity, and health system transformation. The views expressed in this article are those of the authors alone and do not represent the positions of their employers or affiliated institutions.
Background on Discussion with Makaila and Riley
Courtney Bean, OPA President, Charlotte Anderson, OPA President Elect, Sarah Hutchison, OPA CEO and Emily Stevenson, Director of Practice and Policy met with Makaila and Riley on their expanding role in emergency department triage and their need to ensure that there are community resources to re-direct eligible patients to for care. The discussion informed OPA’s interest in publishing this article.
References
1. Tepper, J., et al. (2016). (rep.). Under Pressure: Emergency Department Performance in Ontario. Retrieved April 22, 2026, from https://www.hqontario.ca/Portals/0/documents/system-performance/under-pressure-report-en.pdf.
2. Ocampo-Chan, S. A., & Levy, C. (2025). Rehabilitation in emergency departments: A regional scan and future opportunities. Healthcare management forum, 38(3), 263–272. https://doi.org/10.1177/08404704241292240